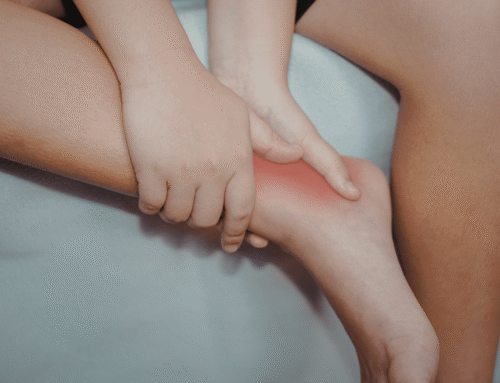
Issues with our tendons can be incredibly frustrating, often starting as a dull ache and progressing to a sharp, limiting pain that stops us from enjoying our daily walks, sports, or even simple household tasks. Whether it is a sudden “tweak” or a grumbling pain that has lasted for months, understanding exactly what is happening under the skin is the first step toward recovery.
In this article, Dr. Simon Nash (Chiropractor) discusses the crucial differences between tendonitis and tendinopathy, explaining how these conditions develop and how a multi-modal chiropractic approach can help restore function.
Medical Disclaimer: The information provided in this article is for general knowledge and informational purposes only and does not constitute medical advice. It is essential to consult with a qualified healthcare professional for a formal diagnosis and personalised treatment plan.
Table of Contents
- What is the Difference?
- Understanding Tendonitis (The Inflammatory Phase)
- Understanding Tendinosis (The Degenerative Phase)
- The Role of Tendinopathy as an Umbrella Term
- How Chiropractic Care Can Help
- Frequently Asked Questions (FAQs)
- Book a Consult with Our Chiro Brisbane
- References
- Video Transcript
What is the Difference?
When a patient walks into our Brisbane clinic clutching a sore shoulder or a painful Achilles, they often use the term “tendonitis.” However, clinical research and modern sports medicine have shifted our understanding of these injuries.
“One of the questions we often get asked at the clinic is what’s the difference between tendonitis and tendinopathy?” notes Dr. Nash. While they sound similar, the biological processes occurring in the tissue are quite different, which means the treatment approach must be tailored accordingly.
Understanding Tendonitis (The Inflammatory Phase)
Tendonitis is characterised by acute inflammation. This is typically the body’s immediate response to a sudden change in activity level or a specific traumatic event.
“Tendonitis is actual acute inflammation or irritation to a tendon caused by repetitive movements or trauma, acute trauma,” Dr. Nash explains. When you have tendonitis, the area is often red, swollen, and warm to the touch. This classic inflammatory response is the body attempting to protect the area, but it results in significant pain and loss of range of motion.
Common examples include:
- Lateral Epicondylitis (Tennis Elbow): Inflammation of the tendons on the outside of the elbow.
- Achilles Tendonitis: Often seen in runners who suddenly increase their mileage.
Understanding Tendinosis (The Degenerative Phase)
If a tendon issue isn’t addressed, or if the tendon is subjected to chronic, low-level stress over a long period, it may move into a state of tendinosis.
“Tendinosis is where you have a non-inflammatory degeneration of the tendon,” says Dr. Nash. “Sometimes you’d see that in more chronic conditions or with certain health conditions as well. Some medications cause that.”
Unlike tendonitis, tendinosis does not involve inflammatory cells. Instead, the collagen fibres that make up the tendon begin to break down and become disorganised. Research published in the International Journal of Molecular Sciences indicates that chronic tendinopathy involves a failure of the normal healing response, leading to “angiofibroblastic hyperplasia” essentially, the tendon structure becomes weaker and less elastic (D’Addona et al., 2017)
“In the clinic, we often see that patients who think they have ‘recurrent’ tendonitis actually have tendinosis,” observes Dr. Simon Nash. “The tissue has changed at a structural level, and we need to focus on rebuilding that strength rather than just ‘cooling down’ inflammation.”
The Role of Tendinopathy as an Umbrella Term
To avoid confusion between inflammation and degeneration, the medical community uses the term “Tendinopathy” to cover all bases.
“Tendinopathy is the umbrella term that we use to describe any problem with a tendon,” Dr. Nash clarifies. “It could be a tendonitis or it could be tendinosis… It’s basically an umbrella term that we use to describe problems with tendons, whether they’re inflammatory or whether they’re degenerative.”
By using this term, your practitioner can acknowledge that your tendon is painful and dysfunctional without necessarily pigeonholing it into a specific stage until a thorough physical assessment is performed.
How Chiropractic Care Can Help
At Our Chiro Brisbane, our approach to tendon issues is holistic. We don’t just look at the spot that hurts; we look at the biomechanics of the entire limb. A study in the Journal of the Canadian Chiropractic Association suggests that manual therapy, combined with eccentric exercise, is highly effective for managing various forms of tendinopathy (Southerst et al., 2015)
Our treatment strategies may include:
- Shockwave Therapy: To stimulate healing in chronic degenerative tendons.
- Cold Laser Therapy: This is excellent for reducing the acute pain associated with tendonitis.
- Dry Needling: To release tension in the muscles associated with the affected tendon.
- Sports Chiropractic Adjustments: To ensure the joints above and below the injury are moving correctly, reducing the compensatory load on the tendon.
“Our goal isn’t just to mask the pain with rest,” says Dr. Simon Nash. “We want to load the tendon progressively. By introducing the right amount of stress at the right time, we encourage the collagen fibres to realign and strengthen.”
Frequently Asked Questions (FAQs)
Q1: How do I know if I have tendonitis or tendinosis?A: Generally, tendonitis is acute (recent) and involves swelling/warmth. Tendinosis is chronic (long-term) and often feels stiff in the morning, improving slightly with movement before aching later.
Q2: Should I use ice or heat for tendon pain?A: For acute tendonitis (swelling), ice is usually preferred to reduce inflammation. For chronic tendinosis, heat may help increase blood flow to the degenerative tissue.
Q3: Can I keep exercising with tendinopathy?A: Total rest is rarely the answer. We usually recommend “relative rest” modifying your activity to a level that doesn’t exacerbate the pain significantly.
Q4: How long does it take for a tendon to heal?A: Acute tendonitis may resolve in a few weeks. However, because tendons have a poor blood supply, chronic tendinosis can take 3 to 6 months of consistent rehabilitation to fully remodel.
Q5: Are certain medications responsible for tendon issues?A: Yes, certain antibiotics (like fluoroquinolones) and long-term corticosteroid use have been linked to an increased risk of tendon degeneration or rupture.
Q6: Does chiropractic care involve “cracking” the tendon?A: Not at all. We use soft tissue therapy, laser, and specific exercises for the tendon itself. Spinal or joint adjustments are only used to improve the overall biomechanics of how you move.
Book a Consult with Our Chiro Brisbane
We know how exhausting it is to live with a nagging injury that just won’t go away. It’s more than just a sore elbow or a tight heel; it’s the frustration of not being able to pick up your kids, finish a gym session, or walk through the supermarket without a limp. You feel like your body is letting you down, and the conflicting advice online only adds to the stress.
At Our Chiro Brisbane, we listen. We take the time to figure out whether you are dealing with acute inflammation or long-term degeneration. Our team is here to provide a clear roadmap to recovery so you can stop worrying about your “dodgy” tendon and start moving with confidence again.
Click here to book your initial consultation with Our Chiro Brisbane today, or call 0732570399.
References
- D’Addona, A., Maffulli, N., Formisano, S., & Rosa, D. (2017). Inflammation in tendinopathy. The Surgeon, 15(5), 297–302. https://doi.org/10.1016/j.surge.2017.04.004
- Southerst, D., Yu, H., Randhawa, K., Côté, P., D’Angelo, K., Shearer, H. M., Wong, J. J., Sutton, D., Varatharajan, S., Goldgrub, R., Dion, S., Cox, J., Menta, R., Brown, C. K., Stern, P. J., Stupar, M., Carroll, L. J., & Taylor-Vaisey, A. (2015). The effectiveness of manual therapy for the management of musculoskeletal disorders of the upper and lower extremities: a systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Chiropractic & Manual Therapies, 23(1). https://doi.org/10.1186/s12998-015-0075-6
Video Transcript
What is sciatica and how can chiropractic help? Sciatica is one of the most common low back problems that we see in clinic and around the world. So sciatica is characterised by pain that or newer pain that runs down the leg so it can run from the top of the buttock all the way down to the foot or anywhere in between, and any combination of that. So the most common causes of sciatica are a disc bulge. So that can be, for example, from the lumbar spine the lower lumbar spine. So maybe L5 which is the last lumbar vertebrae. And that can be caused either down one leg or both legs depending on how the disc bulge sits. So you could have a posterior lateral disc bulge, which means it’s just coming out on one side. Or you could have a central one, and the central one would then hit both nerve roots, and the patient would experience sciatic pain, which is like tingling all the way down the leg. Um, that’s a disc bulge. You could have a facet joint pain. So the joints that make up the lumbar spine are called the facet joints. And they can get irrigated as well. And the patient would typically have pain that runs down to their knee, usually stops around their knee, but it can sometimes overflow a little bit lower. Um, you can also have a thing called piriformis syndrome. So the piriformis is a big muscle that sits in the low part of the buttock and it will actually compress the sciatic nerve, and that is called piriformis syndrome. All of these types of causes of sciatica will be treated differently. So we would look at reducing the inflammation in and around the disc. For the disc one, we would reduce the inflammation around the facet joint for the facet joint problem. And we would look at restoring the function of the piriformis muscle for the piriformis one. So we would use a combination for example of needling. We would use some rehabilitation exercises. We would gently mobilise around the spine. We could use some taping methods whether it be kinesis taping or rigid taping. And when patients are in quite a bit of pain, we can also use a pain free laser called a cold laser therapy. And sometimes we use a combination of all those to help restore function with sciatica. With the different causes of sciatica, we will find that there’s different healing times with that or treatment times. So that can range. Sometimes it can be really fast. You could have an irritation that’s gone within a week. You could have an irritation that sometimes takes 6 to 8 weeks to go away. But we want to make sure that that irritation to the nerve and the reason that nerve is being irritated is taken away, or that function is restored.
One of the questions we often get asked at the clinic is what’s the difference between tendonitis and tendinopathy? So tendonitis is actual acute inflammation or irritation to a tendon caused by repetitive movements or trauma? Acute trauma tendinopathy is the umbrella term that we use to describe any problem with a tendon. So it could be a tendon tendonitis or it could be tendinosis. Tendinosis is where you have a non inflammatory degeneration of the tendon. Sometimes you’d see that in more chronic conditions or with certain health conditions as well. Some medications cause that. So tendonitis is the inflammation. Tendinopathy is any describing word or any describing problem with a tendon. So it’s basically an umbrella term that we use to describe problems with tendons, whether they’re inflammatory or whether they’re degenerative.